Common debates in phlebotomy:
What has your experience taught you?
By Alys Bunce (RGN, PGCE) clinical trainer in phlebotomy, travel health and immunisation.
I love teaching (and practising) phlebotomy. Being able to take blood is such a useful skill to have. One will never be out of a job if they can perform it. Afterall, it’s one of the most important diagnostic tools in medicine. I also really enjoy seeing people transform from being utterly-terrified-of-the-prospect, to desperate-to-get-‘stuck-in’. I am really lucky because due to the nature of my role, I gain some good insights into the common debates in phlebotomy that crop up. I hear things all the time about what is happening (or not) in practice. And a lot of the disparities in practice are often simply down to not having enough training.
The WHO Phlebotomy Guidelines https://www.ncbi.nlm.nih.gov/books/NBK138650/ state:
“Before undertaking phlebotomy, health workers should be trained in, and demonstrate
proficiency for, the blood collection procedures on the patient population that will be within
their scope of practice.” (p77)
However, many practising phlebotomists have never completed a formal course.
Although most of the phlebotomy courses that I deliver are introductory ones, it’s not uncommon to see people on them who have already been taking blood for a number of years. This is because many people who practice phlebotomy learned on the job initially. They tend to have watched someone do the procedure a number times, and then dived right in. Over time, their experience has grown and now they now find themselves to have become a proficient blood-taker.
So, the first ‘debate’ topic: “No need for a course if I’m experienced, right?”
My personal feeling, driven by the often-incorrect practises I have seen, is that it’s never too late to do a phlebotomy course. Clinical skills like this one rely heavily on evidence-based practice and being able to justify actions you have taken, especially in such an invasive and potentially dangerous procedure such as this. Therefore, knowing the ‘steps to take’ and the ‘procedure’ is only half the story. The missing link is often rationale.
The WHO Phlebotomy Guidelines https://www.ncbi.nlm.nih.gov/books/NBK138650/ state:
“Standards of safe practice globally should be governed by evidence-based principles. Each phlebotomy service should, within its capacity, ultimately strive to achieve best practices. Health workers should be protected and allowed to work in a safe environment, armed with knowledge that reduces harm to themselves, patients and the community.” (P49)
I have noticed some patterns emerging from the more experienced delegates that join my phlebotomy courses. And I’m always really glad they chose to attend because a lot of uncertainties can be ironed out and reinforced. Experienced delegates themselves often report back that they learned a lot, which is always pleasing to hear when someone feels that they can improve their practice, even after many years of doing it.
Here are my top three ‘hot topic’ areas around which (sometimes quite animated) debates in phlebotomy tend to come up:
- Butterfly or straight needles?
- To wipe or not to wipe?
- To glove or not to glove?
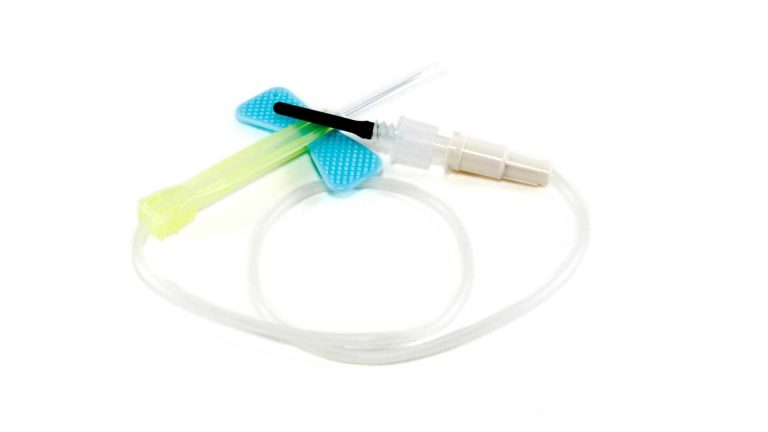
1 How scary can a cute little butterfly be?
This is very much a marmite topic. People seem to either really hate
or really love butterfly needles (or ‘winged infusion devices’ as they
are officially known) with very little in-between. Some people absolutely
refuse to use them, and I’ve been trying to study the reasons why.
Here’s what I’ve found out:
- Cost is quite prohibitive, so if you are in charge of procurement, you won’t like buying the butterflies. As a rough example the cost of a green butterfly needle can be about £1 per unit. The cost of its ‘straight’ equivalent is around 15p. The price goes up again the more safety engineered features that are on the equipment. Massive difference if you are doing a busy bloods clinic with 30 patients a day.
- People often just don’t know how to use them, or when they should be using them, so lack of understanding is sometimes the barrier. People often learn on courses with just a straight needle (maybe some training companies also don’t like the cost?). So, they inevitably feel less confident when they are faced with this new-funny-looking device in practice. For this reason, I always teach my students to use a wide variety of devices, including butterflies, on courses. Dovetail trainers have high standards and no expense is spared when it comes to training supplies.
- Some people report it making the sample-filling process slower. This is because they assume that all butterflies are a smaller girth. Yes, a thinner needle will take a negligible amount of time longer. However, a surprising amount of people don’t realise that butterflies are available in the same widths as a straight needle (E.G. 21G, green) so there is no time or size difference in these circumstances.
- Some just find them Fiddler. Maybe just personal preference...?
What about those who love a butterfly?
Reasons are often because:
- They find them more precise. They make it much easier to get a smaller angle on entry and to target small or very superficial veins. There is definitely a time and a place for a butterfly, and your practise will likely be restricted if you don’t have one or two in stock for certain occasions.
- Less damage can be caused while taking from unpredictable subjects. Despite being the same width in some scenarios (for example, as mentioned, a green butterfly is the same width as a green straight needle – both 21g) they are HALF the length of straight needles so there is less chance of a deep injury if the needle were to be knocked or penetrate further than desired.
- They take blood from hands and feet where ideally, only smaller needles of blue (23G) butterfly size or below should be used. The veins are generally smaller there and more fragile, and it is a more painful location. Butterflies therefore allow for a wider variety of anatomical locations than straight needles.
Butterflies tend to have more options for flash back windows to let you know you’re in the vein – however some straight needles do too. It depends which manufacturer you are using as to what options there are there. Likewise, some butterfly devices don’t have a flashback window either. Flash back windows themselves are a whole other debate by the way. Although very useful for precision and knowing if one is ‘in the vein’, there is controversy over their false negative rates and whether they encourage extra unnecessary attempts… But, I’ll leave that one there for now.
2. Next debate: To wipe or not to wipe?
Oh, this is a VERY heated debate and people get very
animated about this one. Some people glare at me with
the power of a thousand suns when this comes up.
Firstly, all the national guidance on both phlebotomy itself and general infection control guidance, DOES recommend that a cleansing solution containing alcohol (70%) should be used – so please don’t shoot the messenger!!
But why do some people not decontaminate the skin? And not only that, get adamantly defensive when they are recommended to?
Here are the reasons I’ve been given when questioned about not decontaminating skin:
- Money again. And the other practical issue of time; it’s another 30 seconds of wiping and 30 seconds of drying to add to an already-stretched appointment time.
- Applying intramuscular injection guidance (incorrectly) to all needle-in-arm situations. And, yes, injection guidance https://www.gov.uk/government/publications/immunisation-procedures-the-green-book-chapter-4 generally does NOT recommend skin cleansing beforehand.
- Something along the lines of; “I’ve never known a person I’ve taken blood from to get phlebitis or sepsis in 30 years of blood taking”.
- Something else along the lines of; “We have always done it that way so that’s just the way I do it”.
- And statements like; “Wiping can remove good bacteria from the skin surface so it can be WORSE for infection control”.
None of the above reasons convince me to go against the guidance.
And I will tell you why. I’ll take each reason above in turn:
- Money and time are not clinical reasons. They will not stand up in a court of law as reasons for not following clinical recommendations. There is something going wrong in practice if correct timings are not allocated to appointments- or strict budgets are preventing buying appropriate equipment.
- Intramuscular (in the muscle) injections are very different to intravascular (in the vein) procedures. The needle is in a muscle for a much shorter time (no more than 10 seconds generally) and this leaves less time for bacteria to enter the body through the entry site. With phlebotomy one is DIRECTY accessing the venous system, not the muscle or skin tissue where there is more time for the immune system to act on any invaders. Any bacteria entered into a vein will travel around the whole body pretty rapidly. So yes, infection control at the puncture site will definitely reduce the overall impact of bacteria being introduced. Plus, I would question if people always make it habit to go back and check the notes to see if a patient of theirs got sepsis or phlebitis from their venepuncture. Who has time for this? How do they 100% know that they have never caused an infection by not cleansing the skin? In any case, even just one life-threatening sepsis case is not really worth the risk in my humble opinion.
- HOWEVER, blood taking isn’t just about what you put into the body. In fact, the whole essence of it is that you are taking something OUT of it! People often don’t consider that the sample itself needs to be uncontaminated. It has to sit for hours (or days sometimes) before it is processed which gives plenty of time for bacteria to grow and then cause an inaccurate test result.
- As clinical practitioners we should always be prepared to change our practice and go with the latest guidelines. Many things have been done before that we don’t do now upon better evidence. One day the evidence may say not to clean the skin but until it does, I will personally be following the guidance. Any answer that ends with ‘because we’ve always done it that way’ is not good enough. Clinical questions require clinical evidence-based answers. We should always be asking why before doing something to patients– especially if it contradicts guidance.
- Yes, it removes potentially helpful flora and fauna when the skin is cleansed. But it’s a relatively small price to pay for also removing the bad stuff in my humble opinion.
3 The same animated debate occurs around glove use.
Here’s what the WHO guidance
https://www.ncbi.nlm.nih.gov/books/NBK138650/ says:
“Health workers should wear well-fitting, non-sterile gloves when taking blood;
they should also carry out hand hygiene before and after each patient
procedure, before putting on and after removing gloves.” (P50)
The Bloodborne Pathogens standard https://pubmed.ncbi.nlm.nih.gov/34033323/ says:
“Gloves shall be worn when it can be reasonably anticipated that the employee may have hand contact with blood … (and) when performing vascular access procedures.”
And here are the reasons commonly cited for not following this guidance:
- Money (again)
- Can’t feel the veins
- Won’t stop a needle stick injury
Again, money should never be the reason for having to skimp on gold-standards of clinical practice.
Regarding feeling veins – there is no reason why you have to wear gloves to palpate the veins initially. You will (hopefully) be cleaning the skin after that before you get to the stabby bit, and you are not penetrating the skin at this point. After decontaminating the skin, you should not be going back to touch the site anyway, so gloves should not pose a problem. They should, however, be well-fitting as the guidance suggests, or it could indeed make the procedure more fiddly.
And, no, gloves will not stop a needlestick injury. But they will wipe off a large degree of blood on the way in. Hence, significantly reducing the exposure to blood-borne diseases.
The bottom line is this:
Guidance is just that: guidance. Anyone can do anything they please in practice, as long as they are willing to justify their actions in a court of law, or to a disgruntled or harmed patient. But why take the risk of deviating from guidance? Of all the debates I come across in practice, it’s ironic that some of the most common ones aren’t even topics that are up for debate in the literature. Anyway, if everything was a simple as just ‘reading the guidance’, I’d be out of a job. I’m glad I can play a small part in making correct phlebotomy practises a bit easier to understand in a world full of lengthy policy documents and vastly differing opinions.
You might be interested in more topics and questions that come up in practice. Take a look here to sign you or your team up for a phlebotomy course where you will find out answers to other questions and debated topics such as:
- Where exactly are you allowed take blood from?
- Can I take blood from the hand or foot?
- How many ‘goes’ can you have before giving up?
- What age groups am I allowed to take blood from?
- Is my practice discriminatory around people with blood borne diseases? Are there any changes I should make to my practice?
- To pre-vacuum or not with S-Monovettes?
I also enjoy teaching on the travel health and immunisation courses too, where there is usually not a butterfly, an alcohol swab, or a glove in sight.
Hope to see you on one of them some day!
Alys

We need your consent to load the translations
We use a third-party service to translate the website content that may collect data about your activity. Please review the details in the privacy policy and accept the service to view the translations.
